Assault among nursing home workers and frequency and severity of musculoskeletal pain
03/01/2015
Issue #41: Assault among nursing home workers and frequency and severity of musculoskeletal pain
Contributed by Laura Kernan, MS, ProCare Project Manager, CPH-NEW, University of Massachusetts Lowell
Certified Nursing Assistants (CNAs) are the most frequently assaulted group in the United States1, with up to 70% of them reporting assault at work each month. This number is likely underestimated due to under-reporting. In nursing homes, assault may come from residents or a resident’s family member, another staff member, or even a member of the general public. Many studies report psychological issues such as, anger, frustration, self-blame and depression as a result of workplace assault, 2,3 as well as physical reactions such as fatigue, sleep problems and headache. 3, 4
One outcome of workplace assault that has not been explored much is the risk of musculoskeletal problems. A CPH-NEW study, ProCare (Promoting Mental and Physical Health of Caregivers), which evaluates the working conditions and health of nursing home workers, asked nurses and CNAs, "In the past three months, have you been hit, kicked, grabbed, shoved, pushed or scratched by a patient, patient’s visitor, or family member while you were at work?" Workers were also asked whether they had experienced pain or aching in various parts of the body during the preceding three months, and if so to rate its severity. 5
In a baseline survey, almost one-half of participating workers reported being assaulted during the past three months, with 26% reporting one to two assaults and 22% reporting three or more assaults. Importantly, the study also revealed a dose-response relationship for the prevalence of musculoskeletal pain (see figure below). Workers with low back pain also experienced more severe pain when they had been assaulted more often.
Prevalence of musculoskeletal pain, by frequency of recent physical assaults at work5
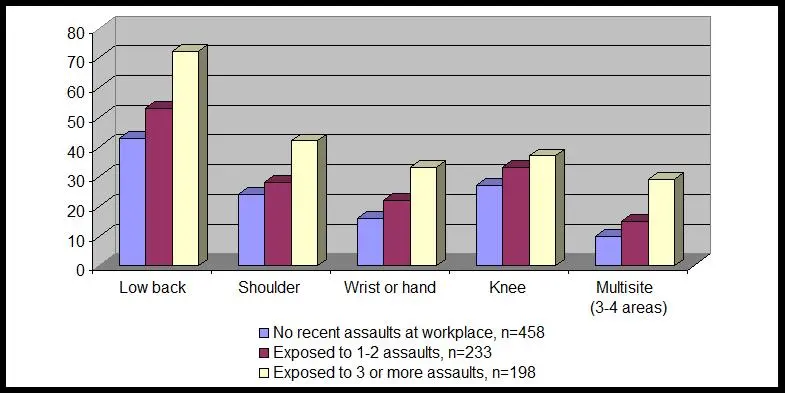
Follow-up at 12 and 24 months after the baseline survey revealed that repeated workplace assaults over time increased musculoskeletal pain occurrence. Workers experiencing assault in all three time periods had the highest rates of continuous pain, depression and pain interfering with work or sleep. 6 More CNA’s experienced these persistent assaults (34%) than did other clinical nursing staff, likely due to the high amount of time that they spend directly with residents.
Health care workers are already at considerable risk from musculoskeletal problems, due to their patient handling responsibilities. These problems may become more severe when stress due to violence (or other causes) slows the healing process. 3, 7 Over time, this could further impact worker productivity and quality of care due to staffing issues. 8
Preventing assault from occurring at work is an important focus of occupational safety in the healthcare sector. Training resources are available from NIOSH (see Resources, below); OSHA recommends several key elements for any assault prevention and control program:
- Talk about it: Set up a company briefing as part of the initial effort to address issues such as preserving safety, supporting affected employees and facilitating recovery.
- Create policies to protect employees: Create and communicate a clear policy that can help prevent violence and supports employee safety and health. Involve nurses and aids in designing and implementing this policy.
- Report it: Encourage employees to promptly report incidents and prohibit reprisals due to reporting.
- Provide resources: Ensure that adequate resources are available and committed to maintain security and support employees in the workplace.9
Laura Kernan, MS, is the ProCare project manager at CPH-NEW. She is also a doctoral student at UMass Lowell in the Department of Work Environment.
References
1. Gates, D.M. The epidemic of violence against healthcare workers. Occup.Environ.Med., 2004; 61: 649-650.
2. Eriksen, W., Tambs K, Knardahl, S. Work factors and psychological distress in nurses' aides: A prospective cohort study. BMC Public Health. 2006; 6.
3. Crofford LJ. Violence, stress, and somatic syndromes. Trauma, Violence, Abuse. 2007; 8:299-313.
4. Hogh A., Sharipova M., Borg V. Incidence and recurrent work-related violence towards healthcare workers and subsequent health effects. A one-year follow-up study. Scand J Public Health. 2008;36(7):706-712.
5. Miranda, H., Punnett L., Gore R., Boyer J., Violence at the workplace increases the risk of musculoskeletal pain among nursing home workers. Occup Environ Med. 2011; 68(1):52-57.
6. Miranda H., Punnett L., Gore RJ. Musculoskeletal pain and reported workplace assault: A prospective study of clinical staff in nursing homes. Hum Factors. 2014(1):215.
7. Finestone H., Alfeeli A., Fisher W. Stress-induced physiologic changes as a basis for the biopsychosocial model of chronic musculoskeletal pain: A new theory? Clin J Pain. 2008; 24:767-775.
8. Besen E., Pransky G. Assessing the relationship between chronic health conditions and productivity loss trajectories. J Occup Environ Med. 2014; 56(12):1249-1257.
9. OSHA. Guidelines for Preventing Workplace Violence for Healthcare and Social Service Workers. https://www.osha.gov/Publications/osha3148.pdf
Resources
NIOSH resources for violence prevention in healthcare sector
OSHA Guidelines for preventing workplace violence for healthcare and social service workers
Guidelines for Preventing Workplace Violence for Healthcare and Social Services Workers
CPH-NEW, a NIOSH Center for Excellence to Promote a Healthier Workforce is a joint initiative by the University of Massachusetts Lowell and the University of Connecticut. CPH-News & Views is a semi-monthly column written by Center researchers on emerging topics related to healthy workplaces. These comments reflect the thoughts of individual Center researchers and do not represent conclusive research summaries. We welcome your responses. Please send to CPHNEW@uml.edu.
CPH News and Views Issue 41
© Copyright 2015 The Center for the Promotion of Health in the New England Workplace (CPH-NEW)
March 2015
